ASTM F2582-20
(Test Method)Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components
Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components
SIGNIFICANCE AND USE
5.1 This test method should be used to evaluate and compare different femoral and acetabular prosthesis designs to assess the damage tolerance under controlled laboratory conditions.
5.2 Although the methodology described attempts to identify physiologically relevant motions and loading conditions, the interpretation of results is limited to an in-vitro comparison between different femoral and acetabular prosthesis designs regarding their ability to resist impingement damage modes (defined in 8.2) under the stated test conditions.
SCOPE
1.1 This test method covers a procedure to simulate dynamic impingement between femoral and acetabular components in a hip replacement; the subsequent qualitative assessment of damage modes (as outlined in 8.2); and, if necessary, quantitative assessment of changes in modular component attachment strength.
1.2 This test method can be used to evaluate impingement between femoral components and the following: single-piece, modular, semi-constrained, bipolar, constrained, or dual mobility acetabular components, manufactured from polymeric, metallic, or ceramic materials.
1.3 The values stated in SI units are regarded as the standard.
1.4 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use.
1.5 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
General Information
- Status
- Published
- Publication Date
- 14-Nov-2020
- Technical Committee
- F04 - Medical and Surgical Materials and Devices
- Drafting Committee
- F04.22 - Arthroplasty
Relations
- Effective Date
- 15-Mar-2015
- Effective Date
- 01-Jun-2014
- Effective Date
- 15-Jan-2012
- Effective Date
- 01-Mar-2011
- Effective Date
- 01-Jun-2010
- Effective Date
- 01-Nov-2009
- Effective Date
- 01-Apr-2009
- Effective Date
- 01-Feb-2009
- Effective Date
- 01-Dec-2008
- Effective Date
- 01-May-2008
- Effective Date
- 01-Jan-2007
- Effective Date
- 01-Mar-2006
- Effective Date
- 01-Oct-2005
- Effective Date
- 01-Jun-2005
- Effective Date
- 10-Aug-2003
Overview
ASTM F2582-20, titled "Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components," establishes laboratory procedures for evaluating the dynamic impingement performance of femoral and acetabular prosthesis designs used in hip replacement systems. This test method provides a standardized approach to assess the damage tolerance and safety of various prosthesis designs under controlled, simulated physiological loading and motion conditions. It is intended to assist manufacturers, researchers, and regulatory bodies in comparing prosthesis designs and understanding their ability to resist impingement and associated damage modes.
Key Topics
- Dynamic Impingement Testing: Simulates the physical interaction, or impingement, between femoral and acetabular hip components during movement to evaluate performance under conditions similar to those experienced in the human body.
- Damage Modes Assessment: Focuses on identifying and characterizing potential failures such as deformation, wear, dislocation, fracture, separation, and loosening. Both acceptable and conditionally acceptable damage modes are addressed to clarify expected findings versus critical failures.
- Component Types and Materials: The method covers single-piece, modular, semi-constrained, bipolar, constrained, and dual mobility acetabular components, and accommodates testing for devices made from polymeric, metallic, or ceramic materials.
- Laboratory Conditions: Testing is performed in vitro, with predetermined compressive loads and angular displacement controls, ensuring standardized and reproducible assessments for comparison across prosthesis designs.
- Worst-Case Scenario Simulation: Procedures are designed to simulate potential worst-case impingement situations, supporting robust safety and performance evaluations.
Applications
ASTM F2582-20 is particularly relevant in the following areas:
- Implant Design Validation: Manufacturers use this standard to validate new or modified hip prosthesis designs before clinical implementation. It provides an essential benchmark for assessing range of motion, impingement risk, and component integrity.
- Quality Control: Ongoing quality assurance and verification for current prosthesis models, ensuring continued resistance to impingement-related damage and regulatory compliance.
- Preclinical Testing and Comparison: Enables direct, laboratory-based comparison between various design options, supporting informed selection and optimization of femoral and acetabular components.
- Regulatory Submissions: Results from this test method can be used in submissions to regulatory agencies, demonstrating compliance with relevant performance and safety criteria.
- Research and Development: Assists in the development of next-generation hip replacement components by providing data that support innovations in locking mechanisms, materials, or geometries with improved impingement tolerance.
Related Standards
Several standards and references are frequently used alongside ASTM F2582-20 for comprehensive hip prosthesis testing and evaluation:
- ASTM F1820 - Test Method for Determining the Forces for Disassembly of Modular Acetabular Devices
- ASTM F2003 - Practice for Accelerated Aging of Ultra-High Molecular Weight Polyethylene after Gamma Irradiation in Air
- ASTM F2009 - Test Method for Determining the Axial Disassembly Force of Taper Connections of Modular Prostheses
- ASTM F2033 and F2091 - Specifications for Total Hip Joint Prosthesis and Acetabular Prostheses
- ISO 7206-1 & 7206-6 - Classification, designation, and endurance property testing for hip joint prostheses
- ISO 14242-1 & 14242-2 - Wear testing and measurement methods for total hip-joint prostheses
- ISO 21535 - Specific requirements for hip-joint replacement implants
Keywords: acetabular prosthesis, femoral component, dynamic impingement, hip replacement, dislocation, laboratory testing, prosthesis evaluation, range of motion, modular component, ASTM hip standards.
Practical Value
By following ASTM F2582-20, stakeholders can ensure the safety, durability, and functional performance of hip replacement systems. Consistent use of this standard supports device reliability, regulatory approval, and, ultimately, improved patient outcomes in orthopedic surgery.
Buy Documents
ASTM F2582-20 - Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components
REDLINE ASTM F2582-20 - Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components
Get Certified
Connect with accredited certification bodies for this standard

BSI Group
BSI (British Standards Institution) is the business standards company that helps organizations make excellence a habit.

TÜV Rheinland
TÜV Rheinland is a leading international provider of technical services.

TÜV SÜD
TÜV SÜD is a trusted partner of choice for safety, security and sustainability solutions.
Sponsored listings
Frequently Asked Questions
ASTM F2582-20 is a standard published by ASTM International. Its full title is "Standard Test Method for Dynamic Impingement Between Femoral and Acetabular Hip Components". This standard covers: SIGNIFICANCE AND USE 5.1 This test method should be used to evaluate and compare different femoral and acetabular prosthesis designs to assess the damage tolerance under controlled laboratory conditions. 5.2 Although the methodology described attempts to identify physiologically relevant motions and loading conditions, the interpretation of results is limited to an in-vitro comparison between different femoral and acetabular prosthesis designs regarding their ability to resist impingement damage modes (defined in 8.2) under the stated test conditions. SCOPE 1.1 This test method covers a procedure to simulate dynamic impingement between femoral and acetabular components in a hip replacement; the subsequent qualitative assessment of damage modes (as outlined in 8.2); and, if necessary, quantitative assessment of changes in modular component attachment strength. 1.2 This test method can be used to evaluate impingement between femoral components and the following: single-piece, modular, semi-constrained, bipolar, constrained, or dual mobility acetabular components, manufactured from polymeric, metallic, or ceramic materials. 1.3 The values stated in SI units are regarded as the standard. 1.4 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use. 1.5 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
SIGNIFICANCE AND USE 5.1 This test method should be used to evaluate and compare different femoral and acetabular prosthesis designs to assess the damage tolerance under controlled laboratory conditions. 5.2 Although the methodology described attempts to identify physiologically relevant motions and loading conditions, the interpretation of results is limited to an in-vitro comparison between different femoral and acetabular prosthesis designs regarding their ability to resist impingement damage modes (defined in 8.2) under the stated test conditions. SCOPE 1.1 This test method covers a procedure to simulate dynamic impingement between femoral and acetabular components in a hip replacement; the subsequent qualitative assessment of damage modes (as outlined in 8.2); and, if necessary, quantitative assessment of changes in modular component attachment strength. 1.2 This test method can be used to evaluate impingement between femoral components and the following: single-piece, modular, semi-constrained, bipolar, constrained, or dual mobility acetabular components, manufactured from polymeric, metallic, or ceramic materials. 1.3 The values stated in SI units are regarded as the standard. 1.4 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use. 1.5 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
ASTM F2582-20 is classified under the following ICS (International Classification for Standards) categories: 11.040.40 - Implants for surgery, prosthetics and orthotics. The ICS classification helps identify the subject area and facilitates finding related standards.
ASTM F2582-20 has the following relationships with other standards: It is inter standard links to ASTM F2091-15, ASTM E4-14, ASTM F2091-01(2012), ASTM F2009-00(2011), ASTM E4-10, ASTM E4-09a, ASTM E4-09, ASTM F1820-97(2009), ASTM E4-08, ASTM F2003-02(2008), ASTM E4-07, ASTM F2091-01(2006), ASTM F2009-00(2005), ASTM F2033-05, ASTM E4-03. Understanding these relationships helps ensure you are using the most current and applicable version of the standard.
ASTM F2582-20 is available in PDF format for immediate download after purchase. The document can be added to your cart and obtained through the secure checkout process. Digital delivery ensures instant access to the complete standard document.
Standards Content (Sample)
This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the
Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
Designation: F2582 − 20
Standard Test Method for
Dynamic Impingement Between Femoral and Acetabular Hip
Components
This standard is issued under the fixed designation F2582; the number immediately following the designation indicates the year of
original adoption or, in the case of revision, the year of last revision.Anumber in parentheses indicates the year of last reapproval.A
superscript epsilon (´) indicates an editorial change since the last revision or reapproval.
1. Scope F2003Practice for Accelerated Aging of Ultra-High Mo-
lecular Weight Polyethylene after Gamma Irradiation in
1.1 This test method covers a procedure to simulate dy-
Air
namic impingement between femoral and acetabular compo-
F2009Test Method for Determining the Axial Disassembly
nents in a hip replacement; the subsequent qualitative assess-
Force of Taper Connections of Modular Prostheses
ment of damage modes (as outlined in 8.2); and, if necessary,
F2033Specification for Total Hip Joint Prosthesis and Hip
quantitative assessment of changes in modular component
Endoprosthesis Bearing Surfaces Made of Metallic,
attachment strength.
Ceramic, and Polymeric Materials
1.2 This test method can be used to evaluate impingement
F2091Specification for Acetabular Prostheses
between femoral components and the following: single-piece,
2.2 ISO Standards:
modular, semi-constrained, bipolar, constrained, or dual mo-
ISO 7206-1Implants for Surgery – Partial and Total Hip
bility acetabular components, manufactured from polymeric,
Joint Prostheses – Part 1: Classification and Designation
metallic, or ceramic materials.
of Dimensions
1.3 The values stated in SI units are regarded as the
ISO 7206-6Implants for Surgery – Partial and Total Hip
standard.
Joint Prostheses – Part 6: Endurance Properties Testing
and Performance Requirements of Neck Region of
1.4 This standard does not purport to address all of the
safety concerns, if any, associated with its use. It is the Stemmed Femoral Components
ISO14242-1ImplantsforSurgery–WearofTotalHip-Joint
responsibility of the user of this standard to establish appro-
priate safety, health, and environmental practices and deter- Prostheses – Part 1: Loading and Displacement Param-
eters for Wear-Testing Machines and Corresponding En-
mine the applicability of regulatory limitations prior to use.
1.5 This international standard was developed in accor- vironmental Conditions for Test
dance with internationally recognized principles on standard- ISO 21535Non-Active Surgical Implants – Joint Replace-
ization established in the Decision on Principles for the ment Implants – Specific Requirements for Hip-Joint
Development of International Standards, Guides and Recom- Replacement Implants
mendations issued by the World Trade Organization Technical
2.3 FDA Document:
Barriers to Trade (TBT) Committee.
21 CFR 888.6Degree of Constraint
2. Referenced Documents
3. Terminology
2.1 ASTM Standards:
3.1 Definitions:
E4Practices for Force Verification of Testing Machines
3.1.1 femoral head—convex spherical bearing member for
F1820Test Method for Determining the Forces for Disas-
articulation with the natural acetabulum or prosthetic acetabu-
sembly of Modular Acetabular Devices
lum.
3.1.2 impingement—the point at which two opposing com-
ponents collide to restrict motion.
ThistestmethodisunderthejurisdictionofASTMCommitteeF04onMedical
3.1.3 locking mechanism—the pieces of various compo-
andSurgicalMaterialsandDevicesandisthedirectresponsibilityofSubcommittee
F04.22 on Arthroplasty. nentsthatcontributetothefixingofonecomponenttoanother.
Current edition approved Nov. 15, 2020. Published December 2020. Originally
approved in 2008. Last previous edition approved in 2014 as F2582 – 14. DOI:
10.1520/F2582-20.
2 3
For referenced ASTM standards, visit the ASTM website, www.astm.org, or Available fromAmerican National Standards Institute (ANSI), 25 W. 43rd St.,
contact ASTM Customer Service at service@astm.org. For Annual Book of ASTM 4th Floor, New York, NY 10036, http://www.ansi.org.
Standards volume information, refer to the standard’s Document Summary page on Available from U.S. Food and Drug Administration (FDA), 10903 New
the ASTM website. Hampshire Ave., Silver Spring, MD 20993, http://www.fda.gov.
Copyright © ASTM International, 100 Barr Harbor Drive, PO Box C700, West Conshohocken, PA 19428-2959. United States
F2582 − 20
3.1.4 range of motion—the effective pattern of motion regarding their ability to resist impingement damage modes
limited by impingement. In one plane this is measured from (defined in 8.2) under the stated test conditions.
one impingement point to the opposite impingement point.
6. Apparatus for Impingement
3.1.5 The following classification by degree of constraint is
suggested for all total joint prostheses, including total hip
6.1 One axis shall be capable of applying a constant
replacementsystemsbasedontheconceptsadoptedbytheU.S. compressive load force for static loading.
Food and Drug Administration (21 CFR 888.6; see 2.3).
6.2 Three motion axes shall be capable of controlling and
3.1.5.1 Constrained—A “constrained” joint prosthesis is
monitoring angular displacement.
used for joint replacement and prevents dislocation of the
6.3 The equipment may be electromechanical,
prosthesis in more than one anatomic plane and consists of
servohydraulic,orother,aslongasitmeetstherequirementsof
either a single, flexible, across-the-joint component or more
Practices E4 for force verification.
than one component linked together or affined.
3.1.5.2 Semi-Constrained—A “semi-constrained” joint
6.4 The compressive load shall be applied through fixturing
prosthesis is used for joint replacement and limits translation
that allows for the separation of the acetabular prosthesis from
and rotation of the prosthesis in one or more planes via the
the femoral prosthesis during the impingement test. See Fig. 1
geometry of its articulating surfaces. It has no across-the-joint
for the test principle. The acetabular prosthesis is allowed to
linkage.
move freely in the horizontal plane but is constrained for
3.2 Definitions of Terms Specific to This Standard:
rotation around the load axis. For hip simulators that do not
3.2.1 compressive load—the force directed normal to the
meet these requirements, the deviations from the standardized
entry diameter of the acetabular prosthesis (see ISO 7206-1).
test setup shall be justified.
NOTE 1—For dual mobility components, the mobile component might
4. Summary of Test Method
be fixated by means of a rotational stop to allow for impingement testing.
4.1 Femoral and acetabular components are evaluated for
fatiguefracture,deformation,delamination,wear,andchipping
7. Sampling and Test Specimens
(ceramiccomponents)underdynamicimpingementconditions.
7.1 All acetabular and femoral components shall be repre-
Modular acetabular prosthesis designs should be evaluated for
sentative of implant quality products. This shall include any
additional damage mechanisms affecting any component or
sterilizationprocessesifthesterilizationmayaffecttheresults.
locking mechanism. Examples of damage modes for modular
7.2 Worst-case specimen(s) shall be determined and justi-
acetabular prosthesis designs include dissociation and loosen-
fied for all conditionally acceptable damage modes (see 8.2).
ing of any component or locking mechanism, or both.
The worst-case specimen(s) may vary by damage mode.
4.2 This test method can be used to evaluate dynamic
Ensure all components in the test are considered, including
characteristics.Various joint reaction forces and impingements
aspects like head offset, stem geometry, surface finish, and
can be applied in order to simulate known clinical conditions.
materialandacetabularcomponent(s)geometry,surfacefinish,
and material. Deformation and wear of components may occur
5. Significance and Use
during testing, and if so, will be continually changing with the
5.1 This test method should be used to evaluate and com-
potential of accentuated change at the times of component
pare different femoral and acetabular prosthesis designs to
repositioning. In consideration of the unknown geometries,
assess the damage tolerance under controlled laboratory con-
calculation of contact stresses and other stresses in the com-
ditions.
ponents(forexample,stressinlockingmechanismregion)that
5.2 Although the methodology described attempts to iden- are needed for worst-case analysis should consider the as-
tify physiologically relevant motions and loading conditions, manufactured (not deformed) geometry of the components.
theinterpretationofresultsislimitedtoan in-vitrocomparison Consideration of overall worst case for each damage mode
between different femoral and acetabular prosthesis designs should consider how deformation and wear will contribute to
FIG. 1 Principle of the Test Setup
F2582 − 20
overall worst case, and will likely need to be based on
evaluation or experience.
NOTE2—Modelingtheneck-rimcontactusingaFiniteElementMethod
(FEM) to determine maximum stress configuration is one possible
technique to support the worst-case analysis.
NOTE 3—Worst-case considerations may include contact geometry,
materialfinish,thinnestacetabularcomponent(s),componentswithlowest
initial locking strength, components exhibiting direct metal-on-metal
contact, and component materials with lowest strength.
7.3 A minimum of three samples shall be tested.
7.4 Precondition the polymeric specimens according to
Practice F2003 (artificial aging) unless there is evidence that
the polymeric specimens are generally resistant to aging.
NOTE 4—The acetabular and femoral prostheses should have freedom
to move relative to each other in the plane perpendicular to the
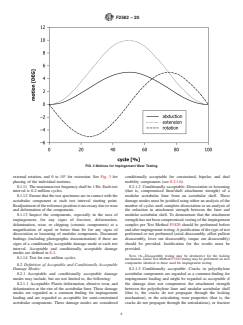
compressiveload.Flexion-extension(FE),abduction-adduction(AA),and FIG. 2 Coordinate System at the Reference Position
internal-external(IE)rotationsarerelativemotionsbetweentheacetabular
and femoral prostheses. Implant in regular (left) and impingement (right)
position.
NOTE 5—Rotation around the load axis is constrained. This can be
angular transformation (Euler angles) is abduction-extension-
achieved by a xy-table.
rotation. For a test frame that does not generate the Euler
NOTE 6—Some simulator designs may allow for xy-translation of the
femoralprosthesis.Inprinciplethissetupissufficientfortestingaccording sequence by its mechanical setup (that is, the extension
tothisstandard,butgreatcaremustbetakentoachievethecorrectloading
actuator is moved by the abduction frame and the rotation
conditions.
actuator is moved by the extension frame), the motions
described in Fig. 3 have to be transformed.
8. Procedure
NOTE 9—The alignment of the cup versus the compressive load is
8.1 Test Procedure:
intended to be constant. The impingement forces generated by simulators
8.1.1 Assemble the acetabular prosthesis according to Test
that do move the cup versus the compressive load force must be analyzed
Method F1820 (if applicable) and the femoral prothesis ac-
to ensure that the loading conditions as described by this standard are
cording to Test Method F2009 (if applicable).
generated.
8.1.2 See Fig. 1 for a schematic representation of the test NOTE10—Theuseofquaternionshasbeenfoundhelpfulforcoordinate
transformation.
setup.
8.1.6 Adjust the simulator actuators for the hip assembly to
NOTE 7—A worst-case test setup for bipolar components is one in
have zero internal/external rotation and zero flexion/extension.
which the outer bipolar component articulation is locked in rotation (A/P,
M/L,andpolaraxes)tosimulatesofttissueimpedingcomponentmobility,
NOTE 11—Computer analysis as well as range of motion testing as
such that there is restricted relative motion between the outer articulation
described by ISO 21535 might support the adjustment of the reference
and the acetabulum.
position.
NOTE 8—Worst-case test setups for dual mobility components include
both (1) locking the outer dual mobility articulation to AP and ML
8.1.7 Apply a constant compressive load of 600 N.
rotations; and (2) allowing the outer dual mobility articulation to freely
8.1.8 Rotate the test assemblies around the center of the
movearoundallaxestoachieveimpingementcontactbetweenthefemoral
femoral head under angular displacement control in abduction
head(skirted)orneckofthefemoralstemandtheacetabularlinerorshell.
motion until impingement in the direction of rotation of these
For (2), impingement at the outer dual mobility articulation is not
test samples occurs. With this starting point and the abduction
intended. This component can be locked to avoid impingement if
necessary. Include in the report which worst-case test setup(s) were
motiondescribedinFig.3,impingementwilloccurthroughout
evaluated and, if one is omitted, a rationale should be provided.
the entire first test cycle.
8.1.3 Mount the acetabular prosthesis with the entry diam-
NOTE 12—The contact conditions shall represent the worst-cast in-vivo
eter plane orthogonal to the direction on the main compressive
situation. Internal/external rotation or flexion/extension of the stem, or
load imposed by the simulator.
both, shall be considered.
NOTE 13—Computer models may be used to evaluate the worst-case
8.1.4 Mount the femoral prosthesis separately, such that the
impingement.
simulator actuators allow for relative motion with the acetabu-
NOTE 14—Testing of constrained prostheses will require additional
lar component, providing flexion/extension, abduction/
mechanical or electronic systems, or both, to limit the test load to the
adduction, and internal-external rotation. The femoral compo-
compressive load of 600 N.
nent assembly shall consist of a femoral head and stem neck
NOTE 15—If a multi-station test frame with mechanically linked
abduction/adduction is being used, ensure that all liners are meeting
region for the minimum length that may contact the acetabular
impingement conditions when setting up at each interval of testing.
component.
8.1.5 See Fig. 2 for the definition of the coordin
...
This document is not an ASTM standard and is intended only to provide the user of an ASTM standard an indication of what changes have been made to the previous version. Because
it may not be technically possible to adequately depict all changes accurately, ASTM recommends that users consult prior editions as appropriate. In all cases only the current version
of the standard as published by ASTM is to be considered the official document.
Designation: F2582 − 14 F2582 − 20
Standard Test Method for
Impingement of Acetabular ProsthesesDynamic
Impingement Between Femoral and Acetabular Hip
Components
This standard is issued under the fixed designation F2582; the number immediately following the designation indicates the year of
original adoption or, in the case of revision, the year of last revision. A number in parentheses indicates the year of last reapproval. A
superscript epsilon (´) indicates an editorial change since the last revision or reapproval.
1. Scope
1.1 This test method covers a procedure to evaluate acetabular component fatigue, deformation, and wear and femoral head
assembly dislocation under dynamic impingement conditions.simulate dynamic impingement between femoral and acetabular
components in a hip replacement; the subsequent qualitative assessment of damage modes (as outlined in 8.2); and, if necessary,
quantitative assessment of changes in modular component attachment strength.
1.2 This test method can be used to evaluate single-piece acetabular prostheses, modular prostheses, and constrained prostheses
impingement between femoral components and the following: single-piece, modular, semi-constrained, bipolar, constrained, or
dual mobility acetabular components, manufactured from polymeric, metallic, or ceramic materials.
1.3 The values stated in SI units are regarded as the standard.
1.4 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility
of the user of this standard to establish appropriate safety safety, health, and healthenvironmental practices and determine the
applicability of regulatory limitations prior to use.
1.5 This international standard was developed in accordance with internationally recognized principles on standardization
established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued
by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
2. Referenced Documents
2.1 ASTM Standards:
E4 Practices for Force Verification of Testing Machines
E467F1820 Practice for Verification of Constant Amplitude Dynamic Forces in an Axial Fatigue Testing SystemTest Method for
Determining the Forces for Disassembly of Modular Acetabular Devices
F2003 Practice for Accelerated Aging of Ultra-High Molecular Weight Polyethylene after Gamma Irradiation in Air
F2009 Test Method for Determining the Axial Disassembly Force of Taper Connections of Modular Prostheses
F2033 Specification for Total Hip Joint Prosthesis and Hip Endoprosthesis Bearing Surfaces Made of Metallic, Ceramic, and
Polymeric Materials
F2091 Specification for Acetabular Prostheses
This test method is under the jurisdiction of ASTM Committee F04 on Medical and Surgical Materials and Devices and is the direct responsibility of Subcommittee
F04.22 on Arthroplasty.
Current edition approved April 1, 2014Nov. 15, 2020. Published April 2014December 2020. Originally approved in 2008. Last previous edition approved in 20082014
as F2582 – 08.14. DOI: 10.1520/F2582-14.10.1520/F2582-20.
For referenced ASTM standards, visit the ASTM website, www.astm.org, or contact ASTM Customer Service at service@astm.org. For Annual Book of ASTM Standards
volume information, refer to the standard’s Document Summary page on the ASTM website.
Copyright © ASTM International, 100 Barr Harbor Drive, PO Box C700, West Conshohocken, PA 19428-2959. United States
F2582 − 20
2.2 ISO Standards:
ISO 7206-1 Implants for Surgery – Partial and Total Hip Joint Prostheses – Part 1: Classification and Designation of Dimensions
ISO 7206-6 Implants for Surgery – Partial and Total Hip Joint Prostheses – Part 6: Endurance Properties Testing and
Performance Requirements of Neck Region of Stemmed Femoral Components
ISO 14242-1 Implants for Surgery – Wear of Total Hip-Joint Prostheses – Part 1: Loading and Displacement Parameters for
Wear-Testing Machines and Corresponding Environmental Conditions for Test
ISO 14242-2 Implants for Surgery – Wear of Total Hip-Joint Prostheses – Part 2: Methods of Measurement
ISO 21535 Non-Active Surgical Implants – Joint Replacement Implants – Specific Requirements for Hip-Joint Replacement
Implants
2.3 FDA Document:
21 CFR 888.6 Degree of Constraint
3. Terminology
3.1 Definitions:
3.1.1 component separation—the disruption of a connection between components. May be stable or unstable.
3.1.2 dislocation—the loss of normal physical contact between opposing components, usually indicated by large separation and
a loss of stability.
3.1.1 femoral head—convex spherical bearing member for articulation with the natural acetabulum or prosthetic acetabulum.
3.1.2 impingement—the point at which two opposing components collide to restrict motion.
3.1.5 joint reaction force—the force directed normal to the entry diameter of the acetabular prosthesis (see ISO 7206-1).
3.1.3 locking mechanism—the pieces of various components that contribute to the fixing of one component to another.
3.1.4 range of motion—the effective pattern of motion limited by impingement. In one plane this is measured from one
impingement point to the opposite impingement point.
3.1.8 subluxation—partial dislocation.
3.1.5 The following classification by degree of constraint is suggested for all total joint prostheses, including total hip replacement
systems based on the concepts adopted by the U.S. Food and Drug Administration (21 CFR 888.6; see 2.3).
3.1.5.1 Constrained—A “constrained” joint prosthesis is used for joint replacement and prevents dislocation of the prosthesis in
more than one anatomic plane and consists of either a single, flexible, across-the-joint component or more than one component
linked together or affined.
3.1.5.2 Semi-Constrained—A “semi-constrained” joint prosthesis is used for joint replacement and limits translation and rotation
of the prosthesis in one or more planes via the geometry of its articulating surfaces. It has no across-the-joint linkage.
3.2 Definitions of Terms Specific to This Standard:
3.2.1 compressive load—the force directed normal to the entry diameter of the acetabular prosthesis (see ISO 7206-1).
4. Summary of Test Method
4.1 Acetabular prostheses Femoral and acetabular components are evaluated for fatigue, deformation, and wear under
repeatedfatigue fracture, deformation, delamination, wear, and chipping (ceramic components) under dynamic impingement
conditions. Modular acetabular prostheses prosthesis designs should be evaluated for additional failure mechanisms including
Available from International Organization for Standardization (ISO), 1, ch. de la Voie-Creuse, CP 56, CH-1211 Geneva 20, Switzerland, http://www.iso.org.American
National Standards Institute (ANSI), 25 W. 43rd St., 4th Floor, New York, NY 10036, http://www.ansi.org.
McKellop, H. A., “The Lexicon of Polyethylene Wear in Artificial Joints,” Biomaterials, Vol 28, 2007, pp. 5049–5057 (Definition of wear modes).Available from U.S.
Food and Drug Administration (FDA), 10903 New Hampshire Ave., Silver Spring, MD 20993, http://www.fda.gov.
F2582 − 20
separation, loosening, fracture, and deformationdamage mechanisms affecting any component or locking mechanism. Examples of
damage modes for modular acetabular prosthesis designs include dissociation and loosening of any component or locking
mechanism, or both.
4.2 This test method can be used to evaluate dynamic characteristics. Various joint reaction forces and impingements can be
applied in order to simulate known clinical conditions.
5. Significance and Use
5.1 This test method should be used to evaluate and compare acetabular prostheses different femoral and acetabular prosthesis
designs to assess the relative degree of constraint for the prosthesis and the damage tolerance under controlled laboratory
conditions.
5.2 Although the methodology described attempts to identify physiologically relevant motions and loading conditions, the
interpretation of results is limited to an inin-vitro vitro comparison between different femoral and acetabular prosthesis designs
regarding constraint and their ability to resist impingement fatigue, wear, deformation, anddamage modes (defined in
8.2dislocation) under the stated test conditions.
6. Apparatus for Impingement
6.1 One axis shall be capable of applying a constant joint reactioncompressive load force for static loading.
6.2 Three motion axes shall be capable of controlling and monitoring angular displacement.
6.3 The equipment may be electromechanical, servo-hydraulicservohydraulic, or other, as long as it meets the requirements of
Practices E4 and E467for force verification.
6.4 The joint reaction force compressive load shall be applied through unconstrained fixturing that allows for the separation of the
acetabular prosthesis from the femoral prosthesis during the impingement and dislocation test. See Fig. 1 for the test principle. The
acetabular prosthesis is allowed to move freely in the horizontal plane but is constrained for rotation around the load axis. For hip
simulators that do not meet these requirements, the deviations from the standardized test setup shall be justified.
NOTE 1—For dual mobility components, the mobile component might be fixated by means of a rotational stop to allow for impingement testing.
7. Sampling and Test Specimens
7.1 All acetabular and femoral components shall be representative of implant quality products. This shall include any sterilization
processes if the sterilization may affect the results.
7.2 A minimum of three samples shall be tested to determine Worst-case specimen(s) shall be determined and justified for all
conditionally acceptable damage modes (see 8.2the impingement wear. Three additional samples should be used as reference
samples without impingement in order to provide a comparison to the amount of mode 1 ). The worst-case specimen(s) may vary
FIG. 1 Principle of the Test Set-UpSetup
F2582 − 20
by damage mode. Ensure all components in the test are considered, including aspects like head offset, stem geometry, surface
finish, and material and acetabular component(s) geometry, surface finish, and material. Deformation and wear of components may
occur during testing, and if so, will be continually changing with the potential of accentuated change at the times of component
repositioning. In consideration of the unknown geometries, calculation of contact stresses and other stresses in the components (for
example, stress in locking mechanism region) that are needed for worst-case analysis should consider the as-manufactured (not
deformed) geometry of the components. Consideration of overall worst case for each damage mode should consider how
deformation and wear that would otherwise occur if the primary samples were not impinging.will contribute to overall worst case,
and will likely need to be based on evaluation or experience.
NOTE 2—Modeling the neck-rim contact using a Finite Element Method (FEM) to determine maximum stress configuration is one possible technique to
support the worst-case analysis.
NOTE 3—Worst-case considerations may include contact geometry, material finish, thinnest acetabular component(s), components with lowest initial
locking strength, components exhibiting direct metal-on-metal contact, and component materials with lowest strength.
7.3 A minimum of three samples shall be tested.
7.4 Precondition the polymeric specimens according to Practice F2003 (artificial aging).aging) unless there is evidence that the
polymeric specimens are generally resistant to aging.
NOTE 4—The acetabular and femoral prostheses should have freedom to move relative to each other in the plane perpendicular to the compressive load.
Flexion-extension (FE), abduction-adduction (AA), and internal-external (IE) rotations are relative motions between the acetabular and femoral
prostheses. Implant in regular (left) and impingement (right) position.
NOTE 5—Rotation around the load axis is constrained. This can be achieved by a xy-table.
NOTE 6—Some simulator designs may allow for xy-translation of the femoral prosthesis. In principle this setup is sufficient for testing according to this
standard, but great care must be taken to achieve the correct loading conditions.
7.4 Precondition the specimens according to ISO 14242-2 (soaking).
8. Procedure
8.1 Test Procedure:
8.1.1 WeighAssemble the acetabular inserts as described by ISOprosthesis according to Test Method F182014242-2. (if
applicable) and the femoral prothesis according to Test Method F2009 (if applicable).
8.1.2 Measure the original (unworn) geometry of the impingement section of the acetabular insert.
8.1.2 See Fig. 1 for a schematic representation of the test setup.
NOTE 7—A worst-case test setup for bipolar components is one in which the outer bipolar component articulation is locked in rotation (A/P, M/L, and
polar axes) to simulate soft tissue impeding component mobility, such that there is restricted relative motion between the outer articulation and the
acetabulum.
NOTE 8—Worst-case test setups for dual mobility components include both (1) locking the outer dual mobility articulation to AP and ML rotations; and
(2) allowing the outer dual mobility articulation to freely move around all axes to achieve impingement contact between the femoral head (skirted) or
neck of the femoral stem and the acetabular liner or shell. For (2), impingement at the outer dual mobility articulation is not intended. This component
can be locked to avoid impingement if necessary. Include in the report which worst-case test setup(s) were evaluated and, if one is omitted, a rationale
should be provided.
8.1.3 Mount the acetabular prosthesis with the entry diameter plane orthogonal to the direction on the main joint reaction force
compressive load imposed by the simulator.
8.1.4 Mount the femoral prosthesis separately, such that the simulator actuators allow for relative motion with the acetabular
component, providing flexion/extension, abduction-adduction,abduction/adduction, and internal-external rotation. The femoral
component assembly shall consist of a femoral head and stem neck region for the minimum length that may contact the acetabular
component.
F2582 − 20
8.1.5 See Fig. 2 for the definition of the coordinate system. The rotation axis is aligned with the neck of the femoral component
and the extension axis is in the frontal plane as shown in Fig. 2 (see X1.8). The coordinate system is stationary in relation to the
acetabular component. The sequence of angular transformation (Euler angles) is abduction-extension-rotation. For a test frame that
does not generate the Euler sequence by its mechanical setup (that is, the extension actuator is moved by the abduction frame and
the rotation actuator is moved by the extension frame), the motions described in Fig. 3 have to be transformed.
NOTE 9—The alignment of the cup versus the compressive load is intended to be constant. The impingement forces generated by simulators that do move
the cup versus the compressive load force must be analyzed to ensure that the loading conditions as described by this standard are generated.
NOTE 10—The use of quaternions has been found helpful for coordinate transformation.
8.1.6 Adjust the simulator actuators for the hip assembly to have zero internal/external rotation and zero flexion/extension.
NOTE 11—Computer analysis as well as range of motion testing as described by ISO 21535 might support the adjustment of the reference position.
8.1.7 Apply a constant joint reaction force compressive load of 600 N.
8.1.8 Rotate a subset of three test assemblies around the center of the femoral head under angular displacement control in
abduction motion until impingement in the direction of rotation of these test samples occurs. With this starting point and the
abduction motion described in Fig. 2, impingement will occur throughout the entire test cycle.
8.1.8 Adjust the other subset (optional) of three assemblies (control samples) in a position which allows for a minimum of 5° of
abduction motion before contactingRotate the test assemblies around the center of the femoral head under angular displacement
control in abduction motion until impingement in the direction of rotation of these test samples occurs. With this starting point and
the abduction motion described in Fig. 3the acetabular component., impingement will occur throughout the entire first test cycle.
NOTE 12—The contact conditions shall represent the worst cast worst-cast in-vivo situation. Internal/external rotation or flexion/extension of the stem, or
both, shall be considered.
NOTE 13—Computer models may be used to evaluate the worst-case impingement.
NOTE 14—Testing of constrained prostheses will require additional mechanical or electronic systems, or both, to limit the test load to the joint reaction
force compressive load of
...







Questions, Comments and Discussion
Ask us and Technical Secretary will try to provide an answer. You can facilitate discussion about the standard in here.
Loading comments...